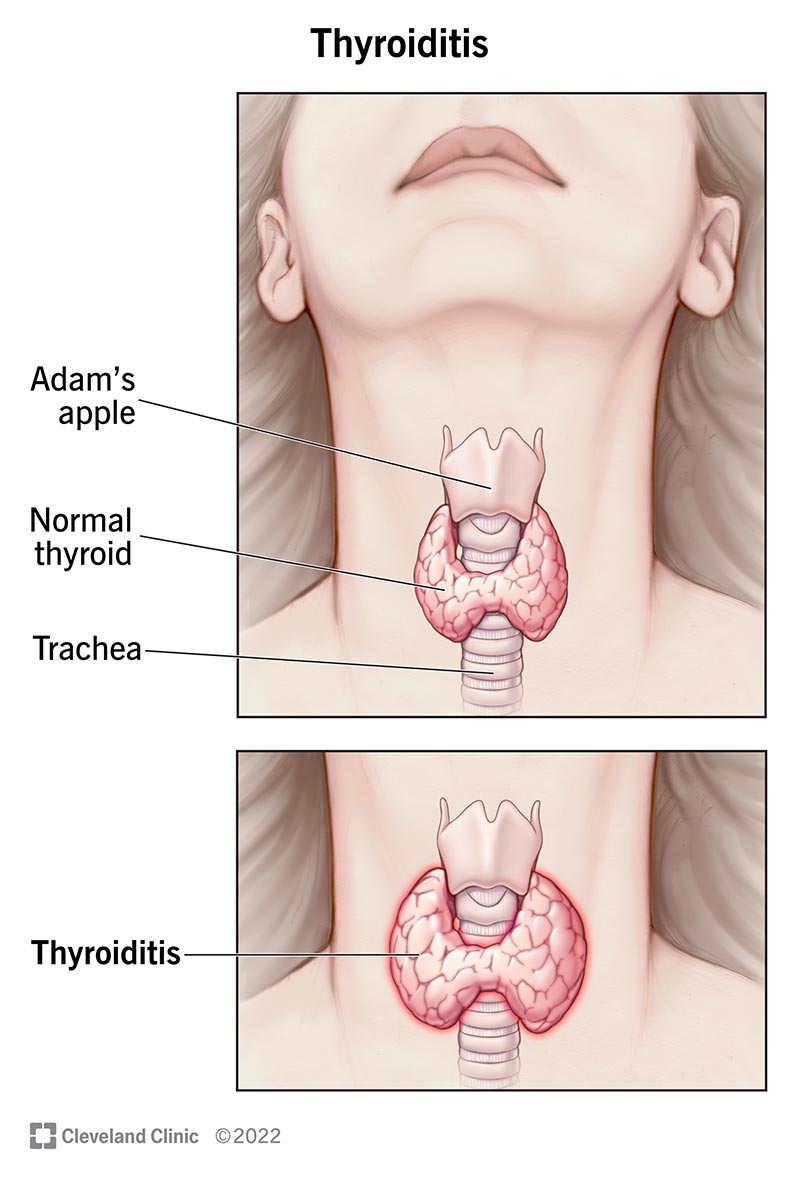
Tiroiditis: Understanding Thyroid Inflammation and Its Diverse Symptoms
The thyroid gland, a small, butterfly-shaped organ nestled at the base of your neck, plays a colossal role in orchestrating your body's most fundamental processes. From regulating energy metabolism and maintaining body temperature to ensuring the normal function of vital organs like the brain, heart, and muscles, its impact is profound. When this crucial gland becomes inflamed, a condition known as tiroiditis, it can disrupt its delicate balance, leading to a spectrum of symptoms that often go unrecognized. Understanding the nuances of an inflamed thyroid is key to recognizing its presence and seeking timely intervention.
What is Tiroiditis? Decoding Thyroid Inflammation
At its core, tiroiditis simply means "inflammation of the thyroid gland." However, this seemingly straightforward definition encompasses a complex group of disorders, each with its own unique triggers, progression, and clinical manifestations. When the thyroid becomes inflamed, its cells can be damaged, leading to an imbalance in the production and release of thyroid hormones into the bloodstream. This disruption can manifest in various ways, sometimes causing an initial surge of hormones (leading to hyperthyroid-like symptoms) and often, a subsequent depletion (resulting in hypothyroid-like symptoms).
The thyroid hormones, primarily thyroxine (T4) and triiodothyronine (T3), are essential for virtually every cell in your body. They regulate how your body uses energy, influencing everything from your heart rate and digestion to your mood and cognitive function. Therefore, when your tiroides inflamada cannot produce or release these hormones effectively, the systemic impact can be widespread and debilitating.
The Many Faces of Tiroiditis: Exploring Different Types
Tiroiditis is not a monolithic condition; rather, it's an umbrella term for several distinct disorders. Recognizing these different types is crucial for accurate diagnosis and tailored treatment. Each form of thyroid inflammation presents a unique challenge and often follows a characteristic pattern:
- Hashimoto's Tiroiditis: This is arguably the most common cause of hypothyroidism in many parts of the world. An autoimmune condition, Hashimoto's involves the immune system mistakenly attacking the thyroid gland, leading to slow, chronic damage and a gradual decline in hormone production. Over time, this chronic inflammation leads to an underactive thyroid.
- Post-Partum Tiroiditis: Affecting women after childbirth, this type of tiroiditis typically presents in two phases. Initially, it can cause a transient period of thyrotoxicosis (high thyroid hormone levels due to stored hormone leakage), followed by a phase of transient hypothyroidism. While often temporary, it's vital for new mothers to be aware of the symptoms as it can impact their well-being during a critical time.
- Subacute Tiroiditis (De Quervain's Tiroiditis): Unlike Hashimoto's, subacute tiroiditis is often characterized by pain in the thyroid gland, sometimes radiating to the jaw or ears. It typically follows a viral infection and also manifests in phases: an initial hyperthyroid-like phase (thyrotoxicosis) as stored hormones leak out, followed by a hypothyroid phase as the gland depletes its reserves, and finally, often a recovery to normal function.
- Drug-Induced Tiroiditis: Certain medications, such as interferon (used to treat hepatitis C and some cancers) and amiodarone (a heart medication), can trigger thyroid inflammation in susceptible individuals. The clinical presentation can vary, ranging from hypothyroid to hyperthyroid states.
- Silent (Painless) Tiroiditis: Similar to post-partum tiroiditis in its biphasic nature (thyrotoxicosis followed by hypothyroidism), silent tiroiditis is an autoimmune condition that occurs in individuals not necessarily linked to childbirth. As its name suggests, it typically does not cause pain in the thyroid gland.
Each of these forms contributes to the overall picture of an inflamed thyroid, and understanding their unique characteristics is the first step toward effective management. For a deeper dive into these specific conditions, you might find our article From Hashimoto's to Post-Partum: Exploring Types of Tiroiditis particularly informative.
Understanding the Symptoms: When Your Tiroides Inflamada Speaks
One of the most challenging aspects of tiroiditis is that there isn't a single symptom exclusive to the condition. Instead, its manifestations often mimic those of other common ailments, making diagnosis tricky. The symptoms depend heavily on whether the inflammation is causing hormone levels to be too high (thyrotoxicosis) or too low (hypothyroidism), and whether the inflammation is acute and painful or chronic and silent.
Symptoms of Thyrotoxicosis (High Hormone Levels):
When the tiroides inflamada rapidly releases stored thyroid hormones, it leads to a state of thyrotoxicosis, which presents symptoms similar to hyperthyroidism. It's important to note the distinction: in thyrotoxicosis due to tiroiditis, the gland isn't *overproducing* hormones; it's simply *leaking* what it has stored. Common symptoms include:
- Anxiety and Irritability: A feeling of being constantly on edge or easily agitated.
- Insomnia: Difficulty falling or staying asleep, leading to chronic fatigue.
- Palpitations and Rapid Heart Rate: A noticeable pounding or racing heartbeat.
- Fatigue: Despite a potentially increased metabolism, many experience persistent tiredness.
- Weight Loss: Unexplained or unintentional weight loss despite a normal or increased appetite.
- Heat Intolerance: Feeling unusually warm or uncomfortable in moderate temperatures.
- Tremors: Fine trembling of the hands.
Symptoms of Hypothyroidism (Low Hormone Levels):
Conversely, if the inflammation causes slow, chronic damage, or if the initial thyrotoxic phase has depleted the gland's hormone stores, the result is often hypothyroidism. This state, sometimes referred to as "thyroid vagueness," reflects a slowing down of bodily functions. Symptoms can include:
- Persistent Fatigue: A profound and unrelenting sense of tiredness.
- Weight Gain: Difficulty losing weight, often accompanied by fluid retention.
- Constipation: Irregular or difficult bowel movements.
- Dry Skin and Hair: Skin may become rough, scaly, or dry, and hair may thin or become brittle.
- Depression and Mood Changes: Feelings of sadness, apathy, or difficulty concentrating.
- Poor Exercise Tolerance: Decreased stamina and increased muscle aches after physical activity.
- Cold Intolerance: Feeling cold even in comfortable temperatures.
- Muscle Aches and Weakness: Generalized body aches or muscle weakness.
The Unique Symptom of Pain:
While most forms of tiroiditis are painless, subacute tiroiditis stands out as the primary cause of thyroid pain. This pain can be localized to the neck, tender to the touch, and may spread to the jaw or ears. This specific symptom often prompts individuals to seek medical attention, offering a clearer diagnostic pathway compared to the more insidious, generalized symptoms of other types.
The non-specific nature of these symptoms means that many cases of thyroid inflammation, particularly hypothyroidism, go undiagnosed. A significant percentage of people with thyroid disorders may be living with symptoms without realizing the root cause. For more detailed information on common symptoms and the challenges of diagnosis, consider reading our article Thyroid Inflammation: Common Symptoms and Undiagnosed Cases.
Causes and Risk Factors for an Inflamed Thyroid
The underlying cause of tiroiditis is typically an "attack" on the thyroid, leading to inflammation and damage to its cells. The majority of tiroiditis cases, particularly Hashimoto's and silent/post-partum tiroiditis, are autoimmune in nature. This means the body's immune system, which is designed to protect against foreign invaders, mistakenly targets its own thyroid tissue.
Other causes and risk factors include:
- Viral Infections: Subacute tiroiditis often follows an upper respiratory tract infection, suggesting a viral trigger.
- Genetic Predisposition: A family history of autoimmune diseases or thyroid disorders can increase the risk.
- Medications: As mentioned, drugs like interferon and amiodarone are known culprits.
- Radiation Exposure: Exposure to radiation, particularly to the neck area, can increase the risk of thyroid inflammation and dysfunction.
- Gender: Women are significantly more prone to thyroid disorders, especially autoimmune forms, than men.
Diagnosis and Management: Addressing Tiroides Inflamada
Diagnosing tiroiditis involves a combination of a thorough physical examination, symptom review, and specific blood tests. Blood tests typically measure thyroid-stimulating hormone (TSH), free T4, and sometimes T3 levels. Additionally, antibody tests (such as anti-TPO and anti-TG antibodies) can help confirm an autoimmune cause like Hashimoto's. Depending on the suspected type, a thyroid ultrasound or a radioactive iodine uptake scan may also be performed to assess the gland's structure and function.
Management of an inflamed thyroid largely depends on the specific type of tiroiditis and the phase of hormone imbalance. For hypothyroidism, thyroid hormone replacement therapy (levothyroxine) is the standard treatment. For the thyrotoxic phase, beta-blockers may be used to manage symptoms like palpitations and anxiety. Pain from subacute tiroiditis can often be alleviated with non-steroidal anti-inflammatory drugs (NSAIDs) or, in severe cases, corticosteroids. It's important to remember that some forms, like post-partum and subacute tiroiditis, can resolve on their own, while others, like Hashimoto's, require lifelong management.
Living with Thyroid Inflammation: Practical Tips and Insights
Living with tiroiditis, whether temporary or chronic, requires proactive management and self-care. Here are some practical tips:
- Regular Medical Follow-ups: Adhere to your doctor's recommendations for blood tests and appointments to monitor your thyroid function and adjust medication as needed.
- Symptom Awareness: Pay close attention to your body and communicate any new or worsening symptoms to your healthcare provider. Keeping a symptom journal can be helpful.
- Balanced Diet: While no specific "thyroid diet" exists, a nutrient-rich, balanced diet supports overall health and well-being, which is crucial when managing a chronic condition. Ensure adequate iodine intake, but avoid excessive amounts, especially if you have autoimmune thyroid disease.
- Stress Management: Chronic stress can exacerbate autoimmune conditions. Incorporate stress-reducing activities into your routine, such as meditation, yoga, mindfulness, or hobbies.
- Adequate Sleep: Prioritize 7-9 hours of quality sleep per night, as fatigue is a common and often debilitating symptom of thyroid dysfunction.
- Gentle Exercise: Regular, moderate physical activity can help manage weight, boost mood, and improve energy levels, but listen to your body and avoid overexertion, especially during periods of high fatigue.
- Support Networks: Connect with others who have similar experiences. Support groups or online communities can provide valuable emotional support and shared wisdom.
Conclusion
Tiroiditis, or an inflamed thyroid, is a nuanced and often misunderstood condition with a wide array of symptoms and underlying causes. From the chronic autoimmune attack of Hashimoto's to the transient post-partum inflammation, its impact on the body's delicate hormonal balance can be significant. Given the non-specific nature of many thyroid symptoms and the high rate of undiagnosed cases, awareness is paramount. If you suspect your thyroid might be inflamed, or if you experience a persistent combination of the symptoms discussed, it is crucial to consult a healthcare professional for accurate diagnosis and appropriate management. Early detection and consistent care are key to mitigating the effects of tiroiditis and maintaining optimal health.